Stuck in the Covid K-Hole
Public health professionals *hate* this one weird trick
There’s a awesome, detailed article in the Washington Post [link] about “super-spreaders”, and what we’ve learned about how Covid-19 spreads through the population. The long and short of it is that the pattern of spread in the virus appears to be very uneven - a few super-spreaders tend to spread the virus far and wide, while most of the infected do not spread it to others at all. There’s not a lot of super-spreading happening outdoors or via casual contact, but a single infectious person in a bar or church can infect dozens more.
This dependency super-spreading turns out to be why Covid-19 has been so hard to suppress. Even countries that thought they had passed the crisis, like Israel [link] or Iran [link], have seen resurgences. However, it turns out to imply a simple strategy for fighting the virus. The virus has a ‘long tail’ of cases who infect very few others and a ‘fat head’ of super-spreading events. Keeping it down requires chopping off the head.
Fooled by Averages
Covid-19 is frequently discussed in terms of R0 or ‘r-naught’, which is how many times an infected person is going to spread the virus. An R0 of 1 means they’ll spread it to one more victim - if R0 is below 1 an epidemic will die out, if it’s above 1 the illness will spread exponentially. You tell two friends, then they tell two friends, then they tell two friends, and then bad things happen. Covid-19 is thought to have an R0 somewhere between 2 and 3.
But here’s the tricky thing - most of those infected with Covid-19 won’t spread it to anyone. Not a single person! Instead, a small number of superspreaders are responsible for a huge amount of spread:
The superspreading individuals, representing 20 percent of the total, were responsible for 80 percent of transmissions. A second group, involving about 10 percent of cases, transmitted the virus to one or two others. The final group, 70 percent, did not infect anyone else at all.
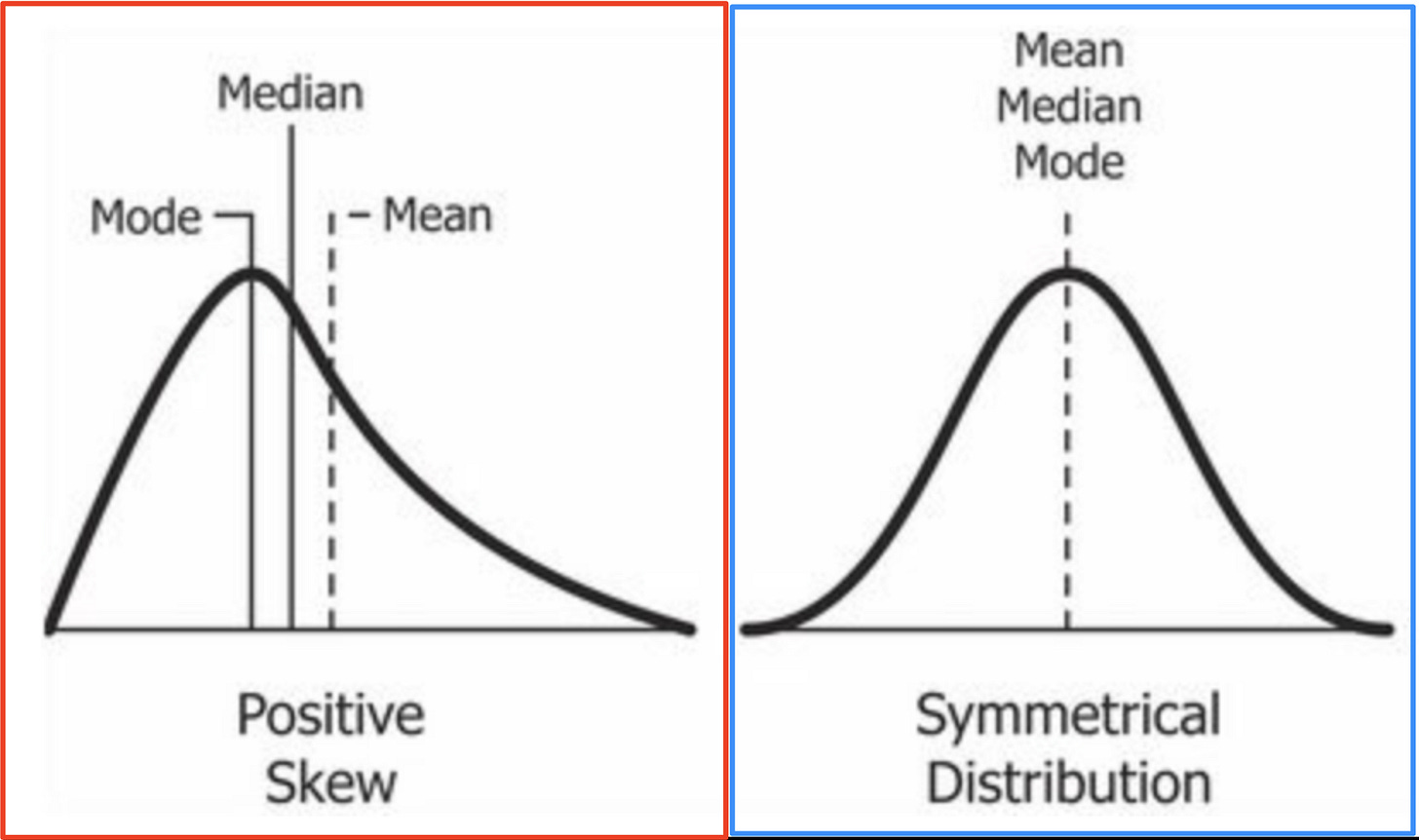
This is in statistical terms a highly skewed distribution. That means one where the mean is quite far from the median - or in qualitative terms, where the average experience does a poor job summarizing what most people experience. Our intuition naturally assumes most averages are describing a world like the one in blue below - when the truth is more like the red one, an ‘average’ can be highly misleading.
Because epidemiologists think about these problems for a living, there’s already a term for how much a disease spreads by super-spreading - k. It was laid out in a 2005 Nature paper [link], which fascinatingly appears to have been motivated by the last novel coronavirus outbreak, the 2003 SARS outbreak. SARS was quite unusual among highly infectious diseases because it appeared to mostly spread via super-spreading. It had an extremely low k of 0.16 while the 1918 flu pandemic had an estimated k of around 1, meaning most victims were equally contagious. SARS really was strange in this respect, which is probably why this notion of k is of such recent vintage.
Covid-19 appears to be even more driven by super-spreading than SARS, with k estimates of around 0.1 [link]. This implies that roughly 10% of infectious people drive around 80% of infections, and in turn it’s why Covid-19 has proven so difficult to address. As the authors of the 2005 paper defining k conclude, “Diseases with high individual variation show infrequent but explosive epidemics after introduction of a single case”. This factor seems to explain why the disease seemed to lie dormant for much of the late spring in states which re-opened early, but took off explosively after it reached sufficient density to spawn a large number of super-spreading events.
K Marks the Spot
Weirdly enough, this is actually pretty encouraging to read. As the authors point out, diseases with high k turn out to be easier to control by focusing entirely on the super-spreading events. To the degree that Covid-19 spread appears to be nearly entirely a product of indoor, high-crowding situations like bars and restaurants, shutting them down should put the disease into reverse. That appears to be what’s driving the plateau in new cases (fingers crossed) in Arizona, Texas, and Florida, which closed bars and restaurants between two and three weeks ago.
Unfortunately, that same message is pretty pessimistic in terms of when life might ‘return to normal’. Normal life involves a lot of indoor, high-crowding situations: bars, schools, restaurants, and offices. Trying to reopen them while the virus is still loose in the population, based on this high-k pattern, will end up feeling normal until it doesn’t anymore. While a lot of life might end up being manageable without further outbreaks, schools, restaurants, and offices are pretty important parts of normal life to go without!
Ultimately, this situation implies that it’s going to be very, very hard to return to normal without stomping out the virus, a cure, or a vaccine. Even in other countries which are doing better than the US today it’d be easy for it to get a foothold undetected due to the super-spreading nature of so many everyday events. Life may get a lot more tolerable than the April lockdowns, but true normal doesn’t appear to be on the horizon anytime soon.
Stay home, stay safe, and don’t be a super-spreader!


This was a super informative. Thanks for the enlightening read, Alex!